Abnormal Bleeding & Fibroids
Fibroids
Uterine fibroids are extremely common. About 40 percent of women over the age of 35 have fibroids, though they often don’t know it. In African-American populations, as many as 70 percent of women over the age of 35 have fibroids. While fibroids are almost always non-cancerous, they can cause pain, heavy bleeding, pelvic pressure and problems during pregnancy.
Fibroids were once the leading cause of hysterectomies in the United States, but many alternative treatment options are now available. Gynecologic specialists with DMC perform the latest minimally invasive and incision-less procedures to remove fibroids. We personalize our approach based on your individual medical needs, as well as your social and lifestyle needs.
Hysteroscopic Myomectomy
An incision-less approach, physicians can use several new techniques to remove fibroids, called a myomectomy. Unfortunately, about 30 percent of the time, the fibroids grow back after all types of myomectomy. The following hysteroscopic myomectomy techniques are available:
- Sonata® - The DMC is the first to provide this incision-free procedure to help relieve debilitating symptoms caused by uterine fibroids. Learn more at Uterine Fibroids Procedure
- MyoSure™ Fibroid Removal — this incision-less procedure safely and effectively removes submucosal fibroids. MyoSure™ is an excellent option for women seeking to reduce heavy bleeding symptoms and preserve uterine form and function.
- Versapoint™ Electrosurgery — this procedure vaporizes fibroids instead of shaving or cutting them. The Versapoint™ System makes it easier for the surgeon to remove the fibroid because there are no tissue pieces left in the uterus that must be withdrawn during the procedure.
- Uterine Ablation — several types of minimally invasive ablation procedure are available and can be very effective in controlling heavy menstrual bleeding from benign causes. By destroying the endometrial lining of the uterus, bleeding can be stopped while leaving the uterus in place.
- Uterine Artery Embolization — also known as uterine fibroid embolization, this minimally invasive procedure blocks the arteries that supply blood to uterine fibroids.
Minimally Invasive Hysterectomy
When a hysterectomy is necessary, our experts can perform a minimally invasive laparoscopic procedure to remove the uterus with just three tiny incisions. This minimally invasive laparoscopic procedure allows physicians to remove the uterus with a quarter-inch incision at the belly button and two half-inch incisions in the lower abdomen. Our minimally invasive approach means you spend less time in the hospital, recover faster and with less pain, and you even have a lower risk of complications. Several different types of minimally invasive hysterectomies are available, including a procedure called Supracervical Hysterectomy. This highly specialized procedure leaves the cervix intact and may result in better bowel, bladder and sexual function compared to a traditional hysterectomy.
Facts about Fibroids
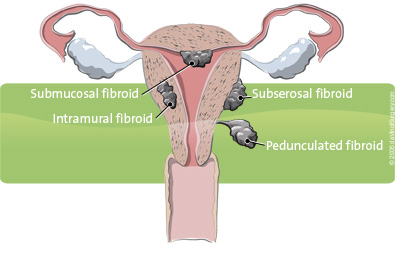
- Fibroids are growths on the smooth muscle of the uterus. They can develop as a single growth or in clusters.
- Fibroids are almost always benign (non-cancerous), but they can cause significant pain, heavy bleeding, pelvic pressure, problems during pregnancy and frequent urination.
- About 40% of women over 35 have fibroids.
- About 70% of African American women over 35 have fibroids.
- African-American women are three times more likely to get fibroids than other women. In African-American women, fibroids also seem to occur at a younger age, grow more quickly, and are more likely to cause symptoms.
- Overweight and obese women are at higher risk of fibroids than other women.
- Fibroids can be as small as a pea or as large as a pumpkin.
- Fibroids are the number one cause of hysterectomies in the United States.
- An estimated 600,000 hysterectomies are performed in the United States annually with about a third of them performed as treatments for fibroids.
- Researchers are not sure what causes fibroids, but it’s clear that fibroids tend to run in families.
- Fibroids tend to stop growing or shrink after menopause.
Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome (PCOS) is a fairly common medical problem affecting approximately 5 to 10 percent of women of reproductive age. It can cause women to have difficulty getting pregnant and can also have serious medical consequences. Though not completely understood, physicians know that if left untreated PCOS may cause cardiovascular disease, diabetes, abnormal growth of the endometrial lining and even endometrial cancer.
As the name suggests, multiple small cysts on the ovaries are the hallmark of Polycystic Ovary Syndrome. For years, doctors believed the cysts were causing the condition. But researchers now believe polycystic ovaries are a sign of the condition, not the cause. In fact, you can be diagnosed with PCOS without having a single cyst on your ovaries.
To be diagnosed with PCOS, you must have at least two of these three symptoms:
- Irregular Menstrual Cycle – most women ovulate on a monthly basis. After ovulation, if you do not get pregnant, your body sheds the lining of the uterus through menstruation. Women who have PCOS usually have irregular ovulation – once every two months, three months or even once a year – and, as a result, irregular menstruation.
- Elevated Levels of the Male Hormone Androgen – for unknown reasons, women with PCOS often have elevated levels of the male hormone androgen. This can be confirmed through laboratory blood tests, but more visible signs include excess body hair, facial hair, acne and even male pattern baldness.
- Polycystic Ovaries – women with PCOS will often have multiple, small cysts on their ovaries. They can be seen with an ultrasound.
In addition to the recognized signs of PCOS, women with the disorder are often overweight. Also, a significant percentage of PCOS patients have abnormal cholesterol levels.
There are a number of ways to treat PCOS. Depending on your individual symptoms, DMC Hutzel Women’s Services physicians often treat the condition with the following therapies:
- Weight Loss – PCOS patients are often obese. This not only poses cardiovascular risks as excess fat (which converts androgen to estrogen) may also lead to increased endometrial thickness, endometrial hyperplasia and endometrial cancer. We often recommend losing weight through exercise and a healthy diet.
- Diabetes Medications (Type 2) – PCOS is often associated with insulin resistance, meaning treatment can include an insulin sensitizer like Metaformin.
- Controlling Cholesterol – with good eating habits, exercise and Metaformin therapy, you may be able to reverse your abnormal cholesterol levels.
- Ovulation Induction Drugs – if you want to get pregnant and are not able to ovulate regularly after two to three months of the above therapies, an ovulation induction drug may be added to the treatment protocol.
- Birth Control Pills – though birth control pills often mask the symptoms of PCOS, oral contraceptives can be a good treatment, as long as you are not trying to get pregnant.


